BILLING CORNER
Billing Corner
- Schedule of Benefits
- Your Billing Process
- Billing Complaints
- Q & A
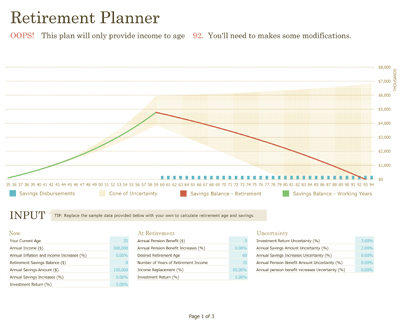
- Financial Planning
- Out of Province Billing - IFHP
- Relativity
Schedule of Benefits (SOB)
MOH OHIP Schedule of Benefits and Fees - January 24, 2022 (Effective November 1, 2021): Download accessible via the MOH website.
COVID19 Income Stabilization
- Ontario Income Stabilization for Physicians As of April 29/20 - nil
- Ontario MOH Loans / COVID-19 Advance Payment Program - download
- Federal Assistance for Small Business Renters - 75% Rent Relief (CECRA) - download
- OMA Summary of COVID-19 Income Stabilization Discussions Across Provinces - download(gated)
Other Resources:
www.CFIB-fcei.ca
Canada's COVID19 Economic Response Plan - download
Ontario Gov't Relief for Small Businesses - download
Federal Programs for Ontario Physicians - download
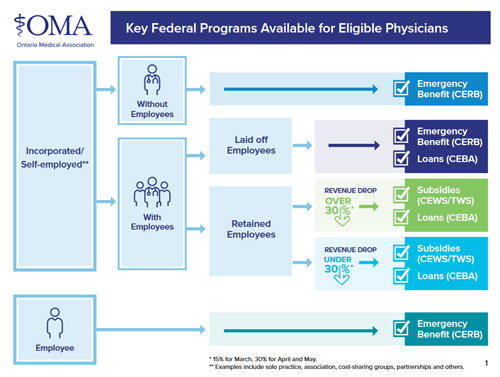
COVID19 CODES
OMA Documents: March 13, 2020; April 13, 2020 - FAQ;
OHIP/MOH Bulletins: March 13, 2020;
2019 MSPC List of Code Increases/Decreases/ New /Deleted
This can be downloaded through your account on the OMA website here . (gated)
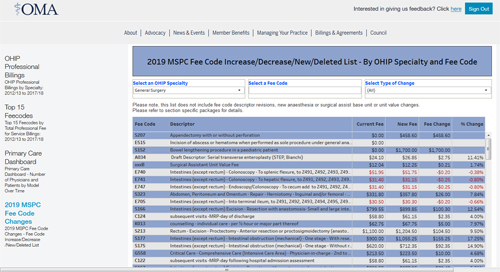
UPDATED: The excerpts below now reflect the non-negotiated, government imposed 1.3% fee reduction that became effective after October 1st 2015 and any subsequent amendments up until Dec.22/15.
GENERAL SURGERY CODES: Selected excerpts from SOB as of Dec.22, 2015 - effective March 1, 2016
- Consultations & Visits - Download PDF (2020)
- Most Responsible Physician (MRP) - Download PDF (2020)
- Counselling - Download PDF
- Travel Premiums - Download PDF
- Assistants Fees - Download PDF
- After-Hours Premiums - Download PDF
- Upper Endoscopy - Download PDF
- Colonoscopy & Sigmoidoscopy - Download PDF
- Stomach - Download PDF
- Colorectal - Download PDF
- Hernia & Abdominal Wall - Download PDF
- Hepatobiliary - Download PDF
- Breast - Download PDF
- Skin & Subcutaneous Tissue - Download PDF
- Appendix - Download PDF (2020)
- Endocrine - Download PDF (2020)
- Vascular - Download PDF (2020)
- Thoracic - Download PDF (2020)
GENERAL SURGERY CODES: Miscellaneous excerpts from SOB
- Morbid Obesity Premium - Download PDF
- Trauma Premium - Download PDF
- Tedious Adhesions Premium - Download PDF
- Nerve Blocks - Download PDF
- TPN Fee - Download PDF
- Varicose Veins - Download PDF
- ICU Visit Premium - Download PDF
- Home Care Forms & Advice - Download PDF
- Physician Telephone Consult - Download PDF
- Criticall (2015-16)- Download PDF
- Multidisciplinary Cancer Conference (2015-16)- Download PDF
- Necrotizing Faciitis (2015-16) - Download PDF
FULL SECTIONS FROM THE SCHEDULE OF BENEFITS
- Section GP: General Preamble - Download PDF
- Section A: Consultations & Visits - Download PDF
- Section J: Diagnostic and Therapeutic Procedures - Download PDF
- Section SP: Surgical Preamble - Download PDF
- Section M: Integumentary System - Download PDF
- Section N: Musculoskeletal System (2016) - Download PDF
- Section R: Haematic and Lymphatic Surgical Procedures - Download PDF
- Section S: Digestive - Download PDF
- Section T: Urogenital & Urinary - Download PDF
- Section U: Male Genital - Download PDF
- Section V: Female Genital - Download PDF
- Section W: Endocrine - Download PDF
- Critical Care - Download PDF
- SOB Numeric Index - Download PDF
- Table of Contents - Download
GENERAL SURGERY CODES: OAGS Billing Summaries
| Colonoscopy Procedure Codes | Diagnostic Code |
|---|---|
| Z491 - FU incomplete polypectomy, large sessile polyp • Or piecemeal or high grade dysplasia • Payable only within 6 months |
546 surveillance |
| Z492 - 5 year FU of a normal colonoscopy • Payable every 5 years after Z499 |
546 surveillance |
| Z493 - 10 year FU of a normal colonoscopy • Payable every 10 years after Z497,Z555 |
546 surveillance |
| Z494 - Very high risk screening - HNPCC, FAP, IBD >10 yrs • Payable within “clinical practice guidelines”(q 1-2yr) |
546 surveillance |
| Z495 - Repeat due to poor prep/ incomplete • No interval limit |
Use Original Code |
| Z496 - Symptomatic • No interval limit |
569 symptoms |
| Z497 - FU+FOBT, +DCBE, +sigmoidoscopy, +CT • Confirmatory - no interval limit |
545 FOBT+ |
| Z498 - Polyp Surveillance Standard Intervals 3 or 5 years • 5 yrs if 1-2 tubular adenoma • 3 yrs if 3+TA, >1cm, villous, any HGD, or Rt. SSA • <3yrs if >10 adenomas • use for colon cancer follow-up at 1, 3, 5 yr intervals |
546 surveillance |
| Z499 - Family History + first scope • 1st degree or two 2nd degree relatives at 40yrs+ (or 10 yrs younger than earliest age of relative's diagnosis) |
547 family history |
| Z555 - Average Risk Screening • Payable at 10-year interval |
548 screening |
Source: MOHLTC Schedule of Benefits (Dec, 2015); Other MOHLTC Schedules-Documents(current).
Your Billing Process
(Scroll to bottom for problem-solving contacts.)- Billing claims are usually submitted by Electronic Data Transfer (EDT) to your local MOHLTC Claims Services Branch.
- Cut-off for submissions is the 18th of each month or next business day if it falls on the weekend (claims received after the 18th may also be processed and included in the same Remittance Advice, not necessarily in the same month)
- Providers must submit claims within 6 months of the date of service (claims submitted beyond this time frame are considered stale-dated and will be rejected to the Error Report)
- If you feel a complicated claim is going to require further documentation, make sure to submit/fax it on the same day as the EDT. Be sure to make a paper trail and get confirmation that they received it. Email confirmation is preferred, but if you call, make note of the time, date and contact person in a journal.
- Cases with multiple procedure codes and duplicate billings are automatically forwarded to a Claims Assessor (other criteria such as billing history may also be used) and will likely be rejected; you'll only be asked to be resubmit the claim with the manual documentation. Save time and delay, and do it the first time!
- Majority of billings are initially assessed through a computer
- Approximately 80% of billings are immediately approved and paid out
- Approximately 20% of billings are not system assessed and are forwarded to Claims Assessors for assessment
- Paid claims will appear on the Remittance Advice (RA)
- Unpaid/rejected claims will appear onthe Claims Error Report or the Remittance Advice with an explanatory code
- Rejected claims appearing on the Claims Error Report MUST BE RESUBMITTED, as they are deleted from the system
- IMPORTANT NOTE: Inquiries regarding overpaid or underpaid claims on the Remittance Advice must be made in writing using the Remittance Advice Inquiry Form. Do not resubmit the claim.
- Claims under review by a Claims Assessor may require further documentation by the physician.
- Fax this documentation to the Ministry office where the physician claims services are performed. Ensure that your billing number is clearly labeled at the top of EACH PAGE of your documentation being faxed. ALSO, remember to flag the claim using your billing software to indicate to the Ministry that special attention is required for that particular claim. Phone/email your local Ministry office if uncertain.
- Once these manual documents are received, your claim is then escalated to an Assessment Officer for further review.
- If the claim and documentation is still too complex or convoluted, it will be further escalated to a Medical Advisor. Once it's been assessed this time, it will appear on the provider's monthly Remittance Advice (RA) either as full, partial or denied payment.
- If the claim has been partially paid or completely denied, the surgeon/provider may appeal this by completing what is called a Remittance Advice Inquiry (RAI) (form#1). This needs to be accompanied with a letter, a note and any other additional documentation which may be of benefit.
- NOTE: Questions to the Medical Advisor should be IN WRITING ONLY. KEEP ALL CORRESPONDENCE for future reference.
- If this additional letter/document supports your appealed claim, then the claim will be adjusted.
- If the Assessment Officer or Medical Advisor stand by their initial rejection, then a response will be sent to the provider/surgeon with an explanation.
- If the surgeon still does not agree, you can appeal one final time with another Remittance Advice Inquiry (RAI) (form#2). This must be accompanied with a formal letter. At this point, it will be escalated a final time to be reviewed/discussed by a panel of three Medical Advisors. All 3 must be in agreement on the assessment. If one of the three advisors does not agree, then the provider's claim is adjusted automatically by default.
- Time Frame: As a rule, it should take about 1 month for each stage - 3 months maximum for the entire process IF you've been diligent in submitting all documentation promptly.
- Stale Billing: This refers to a claim which was not submitted correctly within 6 months of the performance of the procedure. It pertains only to the initial billing and the first response to the Claims Assessor. (After the first response to the Claims Assessor, the 6 month stale billing rule should no longer apply and payment should be made out beyond the 6 months by default, as long as you've complied to their requests in a timely manner.)
- IMPORTANT NOTE: Each physician is responsible for all claims submitted and paid in conjunction with his/her OHIP billing number. So, even if you have a 3rd party submitting your billing, you are still liable for the consequences and fraudulent claims which could jeopardize your license. Be aware of what is submitted under your name and billing number. As such, the MOHLTC recommends that physicians promptly reconcile all claims by reviewing their monthly Remittance Advice and Error Report.
- COMMON ERRORS RESULTING IN NON-PAYMENT: a) missing/illegible 6-digit billing number, clinic's 4-digit ID number, patient's health card number/info, b) documents sent to the wrong district office, or c) requested documentation is not sent along with the submitted/resubmitted claim.
- MOHLTC/OHIP Billing Claims Recommendations: •Contact patients for updated information, • Perform a monthly reconciliation of your Remittance Advice and Error Report, • Keep copies of the Remittance Advice, • Diligently follow up all underpaid/overpaid claims, • Retain all Error Reports until claims are paid, • Make corrections and re-submit claims ASAP, • Ensure new billing staff are properly trained.
Sources: MOHLTC Health Services Branch/Claims Services Branch (OAGS AGM, 2014), OAGS Billing Corner (Issue #36, 2014).
Billing Complaints
- Contact the OAGS Tariff Committee:
Outline your issues in an email to our OAGS office "Attn. Tariff Committee": info@oags.org . - OMA Economics Department
The OMA Economics & Analysis department can also offer billing advisory and mediation: economics@oma.org , 416-599-2580 / 1-800-268-7215. - Ministry of Health/ Service Support Contact Centre (M-F, 8am-5pm) - Phone: 1-800-262-6524 or SSContactCentre.MOH@ontario.ca
Resources:
https://www.health.gov.on.ca/en/pro/programs/ohip/default.aspx
https://www.health.gov.on.ca/en/pro/programs/ohip/docs/billing_questions_help.pdf
Sign up for the MOH/SSCC infobulletin for future billing notices and updated contacts:
https://mailchi.mp/ontario/infobulletin-en
Billing Corner Q&A
Do you have a question for our Tariff Committee?
Online Form: Submit Now
Email us: info@oags.org
Below are some common queries from our members addressed to our OAGS Tariff Committee. Just click on the question to open the respective answer....
Ontario Income Stabilization for Physicians As of April 29/20 - nil
Ontario MOH Loans / COVID-19 Advance Payment Program - download
Federal Assistance for Small Business Renters - 75% Rent Relief (CECRA) - download
OMA Summary of COVID-19 Income Stabilization Discussions Across Provinces - download (gated)
Other Resources:
www.CFIB-fcei.ca
Canada's COVID19 Economic Response Plan - download
Ontario Gov't Relief for Small Businesses - download
Federal Programs for Ontario Physicians - download

OMA Documents: March 13, 2020; April 13, 2020 - FAQ;
OHIP/MOH Bulletins: March 13, 2020;


Surgical Preamble page SP3 paragraphs 10 and 11 in the SOB.
10. When a procedure is performed, a procedural benefit, if listed, should be claimed. Substitution of consultation and/or visit benefits for procedural benefits (except as in paragraph 11), is not in keeping with the intent of the benefit schedule.
11. When a surgical benefit (non-IOP, Complete Care, Fracture or Dislocation) is less than the surgical consultation benefit, and the case is referred, a physician may claim a surgical consultation benefit instead of the surgical benefit. However, to avoid the consultation being counted as such under the Ministry of Health and Long-Term Care limitation rules on the number of consultations allowed per year, the physician should claim the consultation fee under the surgical procedure nomenclature or code. Since the consultation is replacing a procedural benefit which includes the pre- and post-operative and surgical care, no additional claims beyond the consultation should be made.
If the patient was "referred" then I would bill a consult using the referring physician's billing number. For example, a referral from a surgeon at a smaller hospital refers someone they can't operate on, I would bill a consult using their number.
For a transfer, when the decision to operate has already been made (like an appy or a gallbladder), you may only be able to bill a visit, or can try a consult using your colleague's billing number a referring number. GP26 suggests that a patient is transferred, only one assessment fee is billable per admission (so the A035 will negate the C033). If it was an SBO, tics that you later decided to operate on, then a full consult should be billed, (as you will lose 2 days of billing before the surgery).
For post op care, I tried to find the language but couldn't. On GP28 it suggested that if a patient is transferred to your care, subsequent visits should be calculated based on the admission date. I believe this was clarified for us as follows.
So if you are being handed over a post op, you should only bill as if you did the surgery, so only 2 days post op (C032/E083) and day of discharge (C124/E083).
A2. If you are billing an elective visit after 5pm, then no special premiums apply. So, just the 5 units. I'm not sure I can think of a scenario where I would have to call a patient on call after hours. Even in COVID times, it should be able to wait until morning.
S175 (Intestinal obstruction (mechanical)….without resection) pg S18
If elective then bill S332/E757 (umbo hernia repair without resection of strangulated contents.) pg S30
method of repair is not relevant - mesh or primary - in this case.
- Tariff Chair
A. OAGS does not have a policy or recommendation on a "minimum" number of call nor on maintenance of competency. We have a statement regarding "maximum" number of calls. Competency to maintain practice is determined by the College of Physicians and Surgeons of Ontario and this question would be better answered by the CPSO. - OAGS
A. "The College considers a physician’s scope of practice to include the clinical areas in which they have engaged in during the immediate past 2 years. Beyond this 2 year threshold, the College does not set minimums for number of clinical cases, hours, or days spent in a particular practice area in order for a physician to maintain competence. Physicians are expected to keep up with their CPD requirements and any competency requirements stated by institutions in which they work (such as hospitals). Otherwise, we expect physicians to engage in self-reflection with respect to their own competency and limitations, and to report to the College if they have been out of an area of clinical practice for 2 years or more and wish to return." - CPSO, Re-Entry and Change of Scope, Applications and Credentials Department
Part 2: That being said, there is the intent of the code as well. It is outdated to bill all of this in sequence. The spirit of the code (could be) "how far did you get"? So, if you get to the "neocecum" after Right hemi, your call to bill to HF vs. "cecum" but you have essentially completed a full examination of the patients colon. I'm not sure CCO has rectified the OHIP vs. CIRT data for its calculations but has done so for our report cards. That being said, I'm not sure every colonoscopy site has to do this as of yet, does it? I would also suggest billing in sequence. If right colectomy, bill to HF. If sigmoid colectomy or left colectomy, thenbill to cecum, all four codes, but again my opinion. In hopefully the not so distant future, we can rewrite some of these codes to eliminate this issue as well as simplify billing.
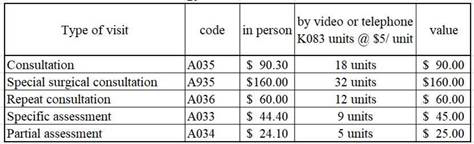
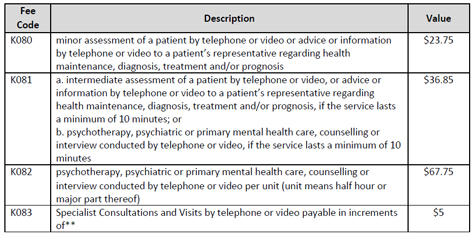
A. The OMA Tariff Department has posted a number of Quick Reference Billing Guides on their website. Below is a table excerpt from the Special Visit Premium Guide:
Source: https://www.oma.org/wp-content/wp-private.php?filename=QRG-SVP-3Aug18.pdf (gated)
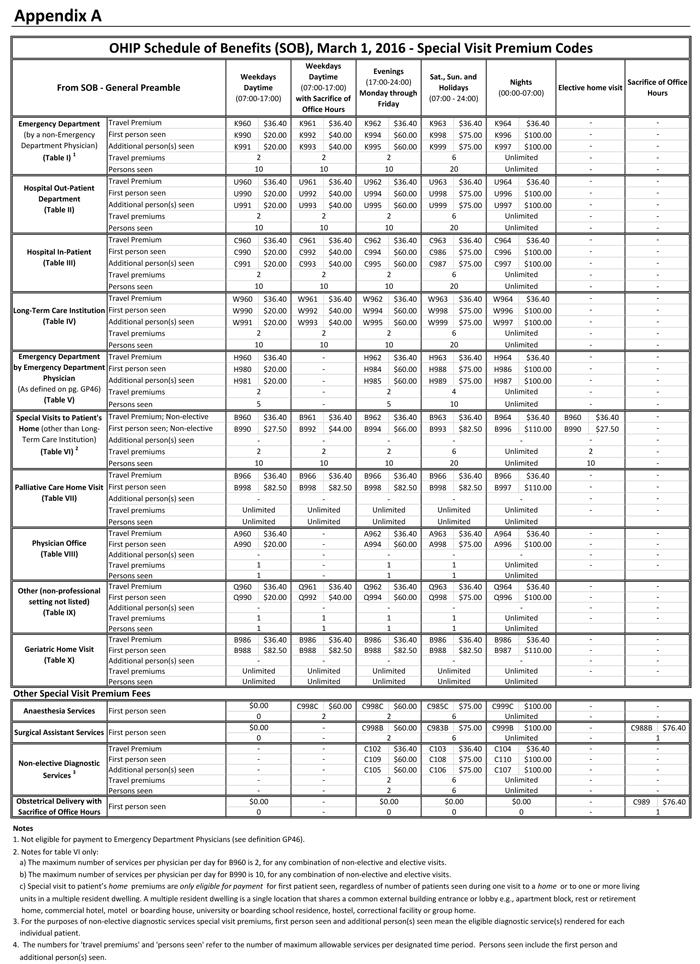
Surgeon - Surgical Preamble, SP6 section 27. If cancelled prior to induction, bill a visit. If cancelled after induction and while scrubbed, bill time plus 6 units.
Assist - General Preamble GP57. Same...Pre-induction: visit. Post and scrubbed: time +6 units. The "Surgical Assist Standby" only applies to a delay longer than 30 minutes, but surgery is performed. If cancelled altogether, then previous rules apply.
For Management of parenteral alimentation: In addition to the common elements, this service includes the specific elements of assessments (see General Preamble GP11). Not to be claimed in addition to hospital visits. G510 Management of parenteral alimentation - physician in charge per visit...21.00, Page J44
"For Management of parenteral alimentation: In addition to the common elements, this service includes the specific elements of assessments (see General Preamble GP11). Not to be claimed in addition to hospital visits."
You have to choose between billing TPN or visits. For day 2 -14 post op, you can’t bill visits, so bill TPN, but after that, visits pay more so bill visits. Some larger centers with shared or group practices designate one member of a group to do surgical nutrition rounds and order TPN but that is stretching things a bit.
Would suggest just billing the visits and forgoing the TPN billings.
TPN = $21
C032+E083 = $40.30
- OAGS Tariff Committee
A. OAGS Tariff Committee Response: These procedures are covered by OHIP and should be billed as such. ...The remuneration is pathetic, but since they are covered, extra billing out of OHIP may put you in jeopardy.... //...If these lumps are "symptomatic" (arguably a broad application here), then (a General Surgeon can) deal with them and bill OHIP. If someone wants it off for COSMETIC reasons, (General Surgeons may not) do it and suggest (the patient) see a Plastic surgeon. It is definitely a grey zone, because it can be done as a "cosmetic" procedure, which the SOB doesn't cover. (Jan.12/18)
A. MOHLTC/OHIP Health Services Branch Response: "Thank you for your question to the Health Services Branch of the Ministry of Health and Long-Term Care (the ministry). We appreciate the time you have taken to write us. Appendix D describes circumstances where removing benign lesions are insured. In general, surgery solely for the alteration of appearance is uninsured. Appendix D describes circumstances where OHIP insures benign skin lesions such as nevi, haemangioma, keratoses, neurofibromata, warts etc. If the physician suspects that a lesion is diseased or malignant, the service to remove the lesion is considered medically necessary whether or not subsequent pathology results shows it to be benign. With prior authorization from the Ministry of Health and Long-Term Care, removal may also be insured if the lesion is very large and disfiguring or if it is to alleviate significant physical symptoms. If the physician is uncertain whether OHIP would consider the service insured, the physician can submit a Request for Prior Authorization for Payment form at http://www.forms.ssb.gov.on.ca/mbs/ssb/forms/ssbforms.nsf/FormDetail?openform&ENV=WWE&NO=014-0691-84." (Jan.22/18)
Interim Federal Health Program (IFHP)
The Interim Federal Health Program, funded by Citizenship and Immigration Canada (CIC), provides limited, temporary coverage of health-care costs to protected persons, including resettled refugees, refugee claimants, certain persons detained under the Immigration and Refugee Protection Act and other specified groups, who are not eligible for provincial or territorial health insurance plans and where a claim cannot be made under private health insurance. The program helps protect public health and public safety, and offers access to urgent or essential health services and products to some of the eligible groups above. The IFHP primarily offers five types of coverage: health care coverage, expanded health care coverage, public health or public safety health care coverage, coverage for the Immigration Medical Examinations, and coverage for detainees. The IFHP provides coverage to eligible beneficiaries, via a contracted claims administrator, through a network of registered health-care providers across Canada. Health-care providers are reimbursed directly for covered services rendered to eligible beneficiaries. - IFHP Program / Medavie Blue Cross
LINKS OF INTEREST:
Out of Province Claim Form for Physician Services: download
Interim Federal Health Program – Information for health-care professionals: download
Information
Handbook
For
Interim
Federal Health
Program
Health-care
Professionals: download
MOHLTC Fact Sheet for Healthcare Providers Re. Syrian Health Care Services:download
Medavie Blue Cross Health Professional Centre: https://www.medaviebc.ca/en/health-professionals
Schedule of Benefits: http://www.health.gov.on.ca/en/pro/programs/ohip/sob/
Syrian Refugee Relocation Aid - As of December 3, 2015...
"The OMA is deeply concerned for those impacted by the incredible disruption in war-torn Syria....The OMA ...encourages members to participate in the Syrian relief effort and will update members as the needs of the new refugee communities become known.
For those interested in providing health care to refugees coming to your community, the memo from Minister Hoskins (https://www.oma.org/Resources/Documents/HoskinsMemoSyrianRefugees20151201.pdf) outlines the province’s plans to ensure health care delivery for those refugees resettling in the province.
The federal government will be covering the costs associated with care for the first year in Canada. Medavie Blue Cross maintains a list of registered providers at http://www.ifhp-pfsi.ca so that private sponsors, clients and others stakeholders can readily identify providers in their community...." - Ontario Medical Association
Other References:
- Medavie Blue Cross - website
- Gov't of Canada IFHP Program - Information for Health Care Professionals - website
- List of IFHP Providers in Ontario- download
Become a Medavie Blue Cross Registered Provider
Refer to the IFHP Information Handbook for Health Care Professionals to find out how to submit the registration form to become a Medavie Blue Cross registered provider.
Determine Client Eligibility
To ensure reimbursement for your services or products by the IFHP, you must verify that a patient is eligible for IFHP with Medavie Blue Cross before providing a service or product each time you see that patient, as a person may cease to be eligible or have their coverage changed at any time.
Before providing a service or product, you can quickly and easily verify your patient’s IFHP coverage:
•Call Medavie Blue Cross at 1-888-614-1880 (08:30 to 16:30 in each Canadian zone); or,
•Log into the secure section of the provider web portal.
•Use these resources to help you navigate the portal and provide services to your patient:
◦Quick Reference Guide – Verify Patient CoverageNote that it takes at least two business days for coverage to be activated in Medavie Blue Cross’ system after it is issued by CIC.
◦IFHP Information Handbook for Health Care Professionals
Submit a claim and receive payment
You must not charge beneficiaries for services or products covered under the IFHP. You must directly bill the IFHP through Medavie Blue Cross. Claims can be submitted electronically via the provider web portal, by mail or can be faxed to 506-867-3841.
Before you provide treatment:
Ask patients if they are eligible for any other private health insurance program or plan that covers the service or product. If the patient has another plan or program, you cannot be reimbursed by the IFHP. Find out more about IFHP coverage types. See the Medavie Blue Cross Provider Portal for benefit grids for each coverage type.
After you provide treatment:
You must ask the beneficiary to sign the claim form before you submit it to Medavie Blue Cross. Submit a claim to Medavie Blue Cross:
•Online:
Submit your claim through the Secure Provider Web portal
•By mail:
Interim Federal Health Program
Medavie Blue Cross
644 Main St. PO Box 6000
Moncton, NB E1C 0P9
•By fax:
506-867-3841
Consult the following Medavie Blue Cross guides for more information on how to submit a claim and receive payment:
•IFHP Information Handbook for Health Care Professionals (PDF, 9.4 MB)
•Quick Reference Guide – Verify Patient Coverage (PDF, 242 KB)
•Secure Web Portal and Electronic Claims Submissions Service Guide (October 2011) (PDF, 125 KB)
•Electronic Dental Claims Quick Reference Guide (PDF, 110 KB)
•Claims Procedures for Point of Sale (POS) Claims Transmissions (PDF, 73 KB)
Resource: Government of Canada Citizen and Immigration - IFHP - website
Relativity
See the Relativity Section here.